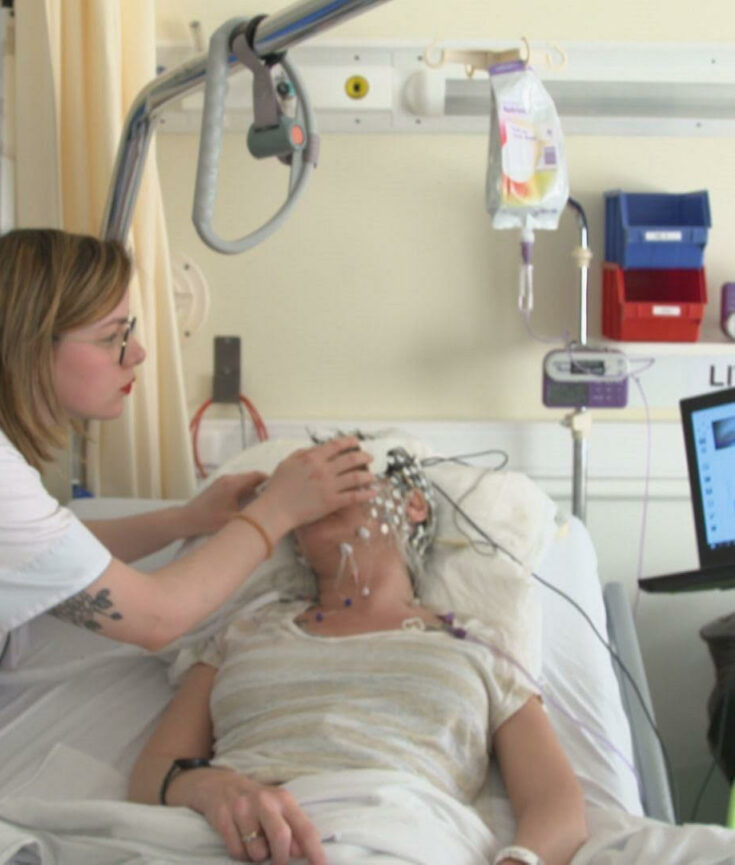
Is a patient responding or not responding to a new drug or treatment? This is an issue for physicians when deciding if a particular patient will benefit from a specific treatment. Each new therapy intervention that is used with the goal of improving someone’s health appears to work well for some individuals that are called responders, whereas for others patients present no effect, i.e. the non-responders.
Predicting what makes a person becoming a responder to a given treatment is still unknown in many cases, and it is an open research question for many existing therapies. Responding to a new treatment might depend on several different factors such as: genetic phenotype, physiology, circadian rhythms, and many, many others. It is interesting to highlight that the responders vs non-responders problem is not only faced by physicians in the medical field. Additionally, dietitians are confronted to people who do not respond to a specific diet, or sport coaches, who see only particular athletes improving after a specifically designed training [4]. This prediction seems of extreme interest in any kind of personalized interventions in order to keep hope, time, and money.

In our Luminous project, a study of consciousness from an electromagnetic point of view, we have developed such a predictor based on the application of machine learning. Our clinical partners at the Coma Science Group in Liege are very interested in actionable decision making tools for patients in minimally conscious state (MCS) ongoing tDCS interventions. We have developed a first prototype of a decision support system, which could help them in their clinical daily practice, to identify responder patients to tDCS by using machine learning algorithms. As you may know trans-cranial direct current stimulation (tDCS) is a non-invasive stimulation technique that modulates the electrical activity of specific regions of the cerebral cortex. There is emerging evidence suggesting that tDCS may promote recovery of consciousness in some minimally conscious state (MCS) patients [1,2]. In the context of MCS patients, such patients are not easy to work with because of their lack of responsiveness and general communication capabilities. Therefore, any help to keep the hope of faster recovery is very welcome!
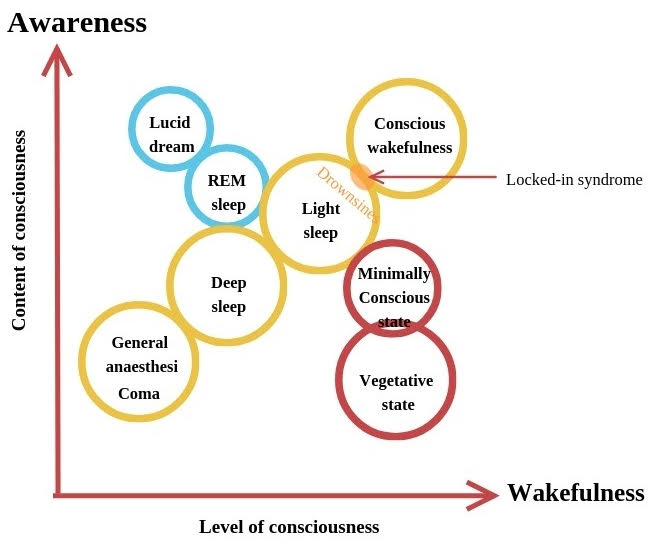
Image 2. Consciousness map
The doctors at the Coma Science Group have applied tDCS to a group of 21 MCS patients. From these, 5 patients showed signs of consciousness recovery after receiving tDCS therapy. You may find this figure too small, but for these patients already is a huge step forward. We have gathered all the data of the patients ,who have gone through tDCS and have had a positive response, to study how to predict patients response to tDCS by using the resting state EEG data collected before the tDCS stimulation was applied to the patients. The goal of this study is to build machine learning (ML) predictive models. Towards achieving this goal, we have built different ML models to classify between responders and non-responder patients. So far our results have shown the potential of such application. With the current small data set of patients, we have achieved an accuracy of 82 % of AUC-ROC at epoch level and accuracy of 94% at patient level AUC-ROC is a an accuracy measure that uses the area under the curve of the receiver operating characteristic curve. It uses the true positive rate (TPR) and false positive rate (FPR) of the classifier to calculate the area under the curve for providing an accuracy measure of the classifier see [5].
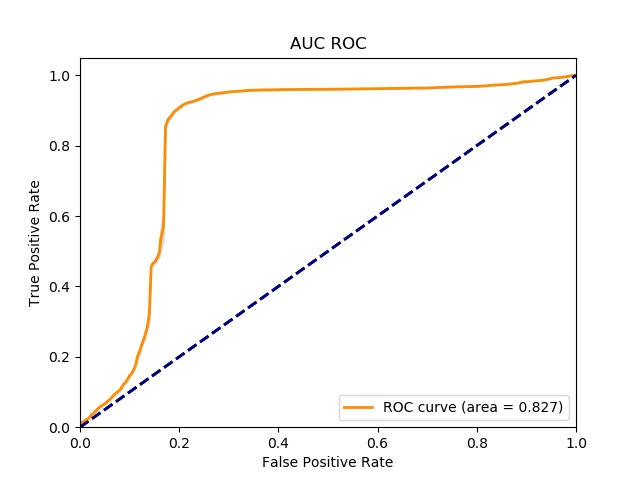
Image 3. Accuracy of the classifier using AUC – ROC
The development of such EEG-based system is enabled by the features of our tDCS devices, which allow for simultaneous stimulation and EEG recording. The EEG can be then used to identify patient response to tDCS therapies. Furthermore the identified EEG markers can be informative on the mechanisms for consciousness recovery after tDCS. In our case low-beta in the frontal-parietal area and alpha in the parietal-occipital area were indicators of such a recovery. This identification is possible because we have provided the interpretability of our ML models to our clinical partners.
In our future work we aim at studying further factors that may influence a patient to become a responder. Our long-term goal is to provide a medical decision support system for physicians to more easily decide whether or not is it worth to apply tDCS to future patients. Stay tuned for news!
References
[1] A. Thibaut, G. Martens, C. Martial, E. Kroupi, A. Soria-Frisch, G. Ruffini, and S. Laureys. Multichannel tDCS of the frontoparietal network in patients with disorders of consciousness: A double blind sham controlled randomized clinical trial. In proceedings of Neuromodulation Conference, 10(4):40, 2017.
[2]Aurore Thibaut, Carol Di Perri, Camille Chatelle, Marie-Aurélie Bruno, Mohamed Ali Bahri, Sarah Wannez, Andrea Piarulli, Claire Bernard, Charlotte Martial, Lizette Heine, Roland Hustinx and Steven Laureys. Clinical Response to tDCS Depends on Residual Brain Metabolism and Grey Matter Integrity in Patients With Minimally Conscious State.
[3] Jungsoo Lee, Ahee Lee, Heegoo Kim, Mina Shin, Sang Moon Yun, Youngjin Jung, Won Hyuk Chang and Yun-Hee Kim. Different Brain Connectivity between Responders and Nonresponders to Dual-Mode Noninvasive Brain Stimulation over Bilateral Primary Motor Cortices in Stroke Patients
[4] Donny M. Camera. Anabolic Heterogeneity Following Resistance Training: A Role for Circadian Rhythm?
[5] Tom Fawcett. An introduction to ROC analysis.
[6] Euronews video article: https://www.youtube.com/watch?time_continue=1&v=zuHBajEm1dQ